|
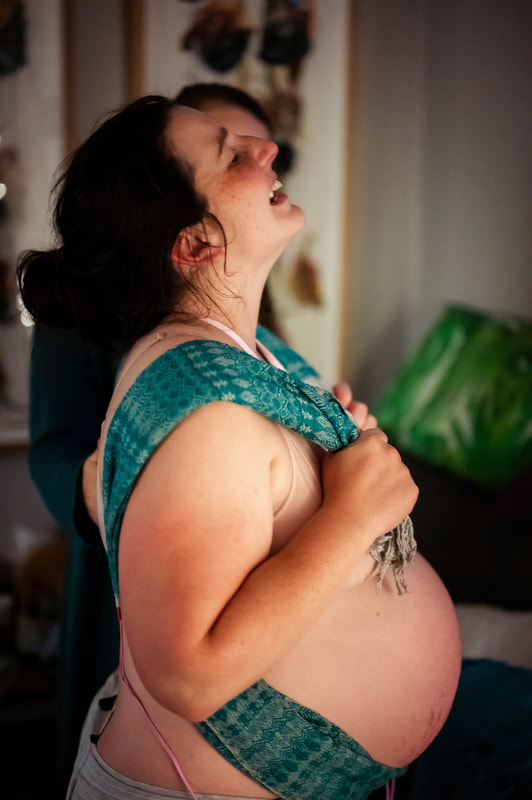
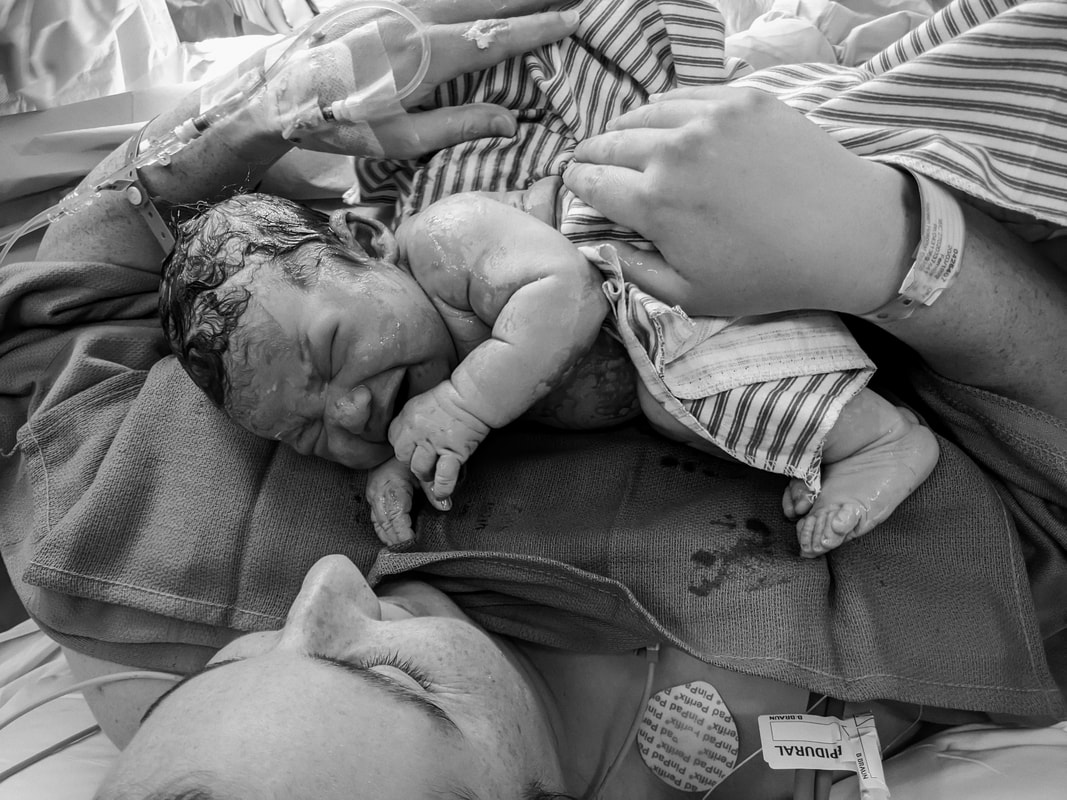
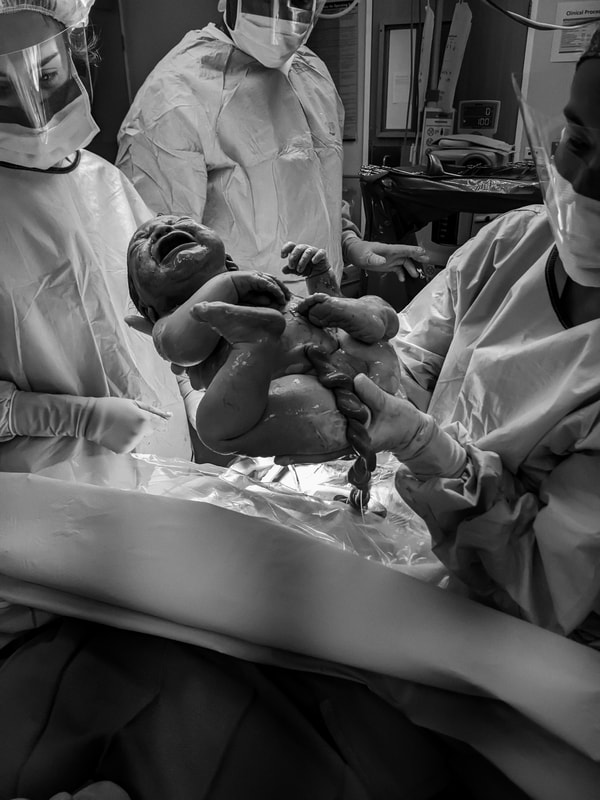
The story of Stella’s journey into the world really begins with her big sister’s. Florence was born via emergency caesarean following a cascade of interventions after an unnecessary and unwanted induction. I started researching VBAC before I’d even left the hospital. After the educational journey I went on, the idea of going to hospital as a healthy woman with a healthy baby to give birth seemed insane and I knew I wanted a HBAC. The evening of 41 weeks, after five weeks of relatively painless prodromal labour, I had my first painful contraction. Another followed within about five minutes, and it was on. Over the next few hours, I set up my birth space while bouncing on a ball, TENS machine on and vocalising strongly with the help of my doula. I laboured about six hours before hitting a wall. My contractions had been feeling good and productive, but a new pain had developed like a thin, tight band pulling from my pelvic bone. I knew instinctively it wasn’t an emergency - just a signal that labour wasn’t progressing as well as it could. I pushed through, moving from the pool, to the toilet, to the lounge room. I couldn’t get relief from the intensity of that band no matter what I tried. After a strong and productive start to labour, I’d felt sure I’d be having a baby before sunrise, so as I noticed the sky lightening through the curtains, my resolve was faltering. My midwife arrived around 7am (my doula and photographer had arrived earlier in the night) and the sound of her keys jangling in her hand as she walked up to the front door made my heart swell with relief. She sat quietly next to me, spoke gently and watched me for a while. I decided on a vaginal exam, hoping to discover why I was stagnating. I was dilated to 7cm, but baby was quite high. My midwife kept her hand still while I had a contraction and informed me that I had a huge bag of waters that was going rock solid when I contracted, which was possibly why baby wasn’t able to descend. She also noticed that bub was pushing against the top of my pelvic bone during a contraction, explaining the tight band of pain I’d been experiencing. I was exhausted, but had a renewed energy with my midwife there and an explanation for how my labour was feeling. We tried a forward leaning inversion, followed by Walcher’s position and something to eat and drink before resting a while. I slept as best I could for a couple of hours, and then treated my neighbours to a show as I trudged the hill down our street in a short house dress, TENS machine wires poking out from behind my bum, adult nappy on to catch the bloody show that was still seeping out of me, mooing with each contraction, and doing abdominal lift and tucks with a rebozo with each surge. Despite everything, my contractions spaced out further as the day went on. I had a hail mary visit to the chiro in the late afternoon before surrendering to a hospital transfer with contractions now fifteen minutes apart. We were fortunate to be allowed two support people, I’m not sure how I would have managed otherwise. Having my midwife felt like having a shield against the system, and we were lucky to be treated with respect and kindness. When we were taken into our birth suite, I appreciated the hospital midwife’s hands-off approach. We requested an artificial rupture of membranes, which hadn’t been safe to do at home but which we hoped would clear the path for my baby’s head to descend. The exam preceding the AROM was awful. The emotional exhaustion was catching me up and I was having to face the reality of the hospital transfer and all that comes with it. I sobbed my way through the VE, tears running down my face as my dear midwife gripped my hand and held her other hand to my cheek and my husband stroked my hair. The hospital midwife broke the waters and she felt the head descend slightly. I laboured for another couple of hours: sitting on the bed, standing and leaning on the bed, even in the shower. I was so exhausted that my legs were barely holding me up any more, but my contractions were so intense that I couldn’t sit through them. I was losing energy to vocalise, which was the only thing keeping me grounded. As strong as they were, they were still ten minutes apart. At twenty-six hours in, and the prospect of labouring for still many more hours, my desperation was mounting. I knew there was a real chance of a repeat caesarean now, and I asked for an epidural, hoping it would relax my body and allow me rest so that I could still give birth to my baby vaginally. I cried as I told my midwife and husband that I couldn’t keep going. I was sad, disappointed, scared and confused. I’d worked so hard for so long with all the confidence that my body and baby knew what they were doing and I just needed to work with them and power through it. Now, I was unravelling alongside my plan for a natural, peaceful water birth at home. Within the hour of getting an epidural, we were recommended a repeat caesarean. The doctor was lovely and respectful. After a frank conversation with my midwife discussing the risks, benefits, and the reality of our situation, I knew the right call was to go to surgery. I watched my delicious, gooey, chunky baby pulled out of my body and flopped straight onto my chest, and I moved her luscious, twisty cord to joyfully confirm my suspicions that she was a girl. We spent a few nights in hospital before returning home and reuniting with my eldest. I’m not alone in reconciling the complexity of a homebirth transfer and caesarean, and to all of us out there, know this: giving birth to a baby at home is not what makes you a homebirther. Our belief in the rite of passage of birth, and the respect for our right to bodily autonomy and informed decision making are what make us homebirthers. I believed so completely in my ability to have my baby at home, processing the fact that I didn’t has been a challenge. One of the hardest parts to accept is that I will never know why she didn’t descend. While I can speculate until the cows come home, I will never know. If I had another baby, I’d plan a HBA2C. I couldn’t walk into a hospital as a healthy woman with a healthy baby to have major abdominal surgery purely because of a couple of scars on my uterus. Plus, I reflect with such fondness on the relationships I developed with my birth team, and the care that they took with my family and me. My eldest still talks about “her friends” and plays midwife with her doctor’s kit. These women have left a lasting impression on us, and I will be forever grateful to them for empowering my journey to becoming a parent for the second time. About Katelyn I’m a married mum of two beautiful girls, Florence and Stella, living in Western Sydney. I used to be a person who said “I love the idea of a homebirth but it’s not for me” until after the birth of my first child when I experienced the maternal health care system and witnessed the way guidelines and policy fly in the face of evidence, and care providers are both inexperienced in assisting with and afraid of physiological birth. My subsequent educational journey has made me an aspiring birth worker and homebirth advocate. I am particularly passionate about supporting women in navigating their next birth after caesarean, and desire for every woman to be empowered with properly informed decision making in their pregnancy, birth, and postpartum. I have since trained as a doula and released a birth after caesarean mentoring program. You can find me at @thenbacguide on instagram or katelynthedoula.com.au
77 Comments
Luaren
11/1/2023 05:02:16 am
Reply
Ann Earnis
2/15/2024 01:53:34 am
HOW I GOT MY HUSBAND BACK WITH THE HELP OF PRIEST WISDOM CONTACT ON WHATS_APP NUMBER +2348124644470
Reply
Virginia Harold
7/14/2024 02:46:31 am
Advice to save your marriage and get your Ex Boyfriend/girlfriend back ,contact [email protected] or WhatsApp +14242983869 for Urgent effective love Spell to get ex lover back or save you marriage fast and his result is 100% guaranteed.
Reply
Love April
1/17/2024 07:52:10 pm
POWERFUL SPELLS CASTER TO HELP BRING BACK SPOUSE 2024 CONTACT [email protected] WhatsApp +1 (502) 512-0989
Reply
Cyril Vivian
2/1/2024 10:13:02 am
Please visit
Reply
Ann
2/15/2024 01:52:17 am
HOW I GOT MY HUSBAND BACK WITH THE HELP OF PRIEST WISDOM CONTACT ON WHATS_APP NUMBER +2348124644470
Reply
Christopher Morris
3/2/2024 06:24:37 am
I met my wife when I was working and living in Alaska. Ever since we got married, it has been all good till she decided to go for a summit in another state where she met someone who became closer to her and eventually he eloped with her. All my efforts to get back home to me was all in vain and her family did their best to reunite us but nothing worked. Just like everyone else, I came in contact with Dr Isikolo and he eventually did wonders and now my wife is back to me. It was revealed that she was hypnotized by the guy who eloped with her. I am glad I never let my emotions get the best of me to have ended my marriage with her. Dr Isikolo is a strong spell caster and trust him when he says the results will manifest just after 48 hours. Contact him now if you need any help email: [email protected] or text him on WhatsApp him on +2348133261196
Reply
Clara Fredrick
3/6/2024 01:47:17 am
I am so happy to share this fantastic testimony of mine. My life has changed round completely in 48hours. I can see myself in the mirror and smile. I have confidence in myself and my abilities for the first time in ages. I have my boyfriend back in my life with the help of Dr Oniha. He said sorry 24 hours after the spell was created. He said he realised that he never really wanted to break up and he could not handle emotional baggage I was carrying around all the time. He said that he thought he was the negative influence on my life and thought it best to leave. He said it was hard that I kept talking about the past all the time. We have both forgiven each other. I have money in my pocket that is my own at last. (My compensation cheque came through. I was told it was months away. I am living proof of what Dr Oniha can do. I thank you so much Dr Oniha for the wonderful thing you did in my relationship. I am so happy now. With your help we were both able to see and speak the truth to each other. I never thought a spell could help a couple before. I am very pleased to contact you and initiate all this to happen. Anyone who has a relationship problem can contact Dr Oniha via email [email protected]. Or his website on http://onihaspells.com
Reply
JACK WAGNER
3/14/2024 04:36:44 pm
Hello everyone I'm JACK WAGNER, I want to testify of the great and powerful spell caster named Dr. ABDUL who brought back my ex who left me and got engaged to another man, We were happy together then She suddenly he just changed, She used to call me every morning and night before going to bed but all that stopped when I call her she yell at me and told me she didn't want to have anything to do with me anymore I was so sad and confused I didn't know what to do then I went online to search on how to get back my ex then I found an article where someone was talking about how the great and powerful Dr. ABDUL helped him and he left his email address I took it and contacted him I told him my problem he only smiled and told me to relax everything will be OK I did everything he asked me to do and he assured me that after 24hrs she will be back, To my greatest surprise the next morning it was my girlfriend she came back kneeling and begging for me to accept her back now we are so happy together now. He can also help you, Email: [email protected] or contact him WhatsApp: +2348108728256
Reply
valetina daniel
3/25/2024 02:06:55 pm
MY MARRIAGE IS SETTLED BY PRIEST LEVENO
Reply
Daniella Gassaway
4/20/2024 12:51:30 am
I'M PREGNANT TODAY ALL BECAUSE OF THIS POWERFUL SPELL CASTER DR UWAIFO SEND HIM A WHATSAPP CHAT:+1(315) 277-2762 I’m Daniella from New York. I came across Dr Uwaifo post and testimony of how he has helped people solve their problems when I was frustrated and depressed looking for help online on what to do to get pregnant after four years of childlessness. I saw great testimonies of his works and how he has put smiles on people’s faces. I contacted him via the number on his page and told him what I was going through, and he told me not to worry that I will carry my children and I claim it. Long story short, he told me what to do and I follow his instructions strictly without missing any words. I was still doing my wifey duties, few months later i got pregnant, i and my husband was so happy we now have a baby not just one but twins after years of trying Dr Uwaifo spell casting turn our situation around. Thank you for putting a smile on our face Dr. Email: [email protected] or whatsapp him: +1(315) 277-2762 or Website; https://druwaifospelltempl.wixsite.com/my-site-1
Reply
Victoria Durham
5/1/2024 03:17:43 am
Hello everyone, my name is Victoria and i live in Houston Texas. Anyone who has lost the faith of having his/her lover back should run to Dr Uwaifo. He's a powerful man and his words are real. This is my testimony. On the 2nd of February 2024, my boyfriend was taking his shower and he left his phone in the room where I was, all of a sudden a multiple text messages came into his phone and i decided to check the text what i saw, i could not believe it, another lady was sending my boyfriend her picture asking my him if he love the picture that she send. Then i reply back to the lady text yes the picture is so hot, her reply again was thank you baby. I wanted to ask my boyfriend about it, but i could not and i was in pain, my heart was beating. I cried that day and i could not stop thinking about the text message, So i went online to search of having my boyfriend back and the first post I saw was Dr Uwaifo how he helped Lily Lopez. I quickly send him a WhatsApp message and Dr reply to me so I cried all my pain to Dr and he told me not to worry that he will bring back my boyfriend to me. That i have to give him 24 hours to cast the love spell. So I waited, the next day my boyfriend came to me himself telling me he was cheating on me but he has ended the relationship with the lady. He asked for forgiveness which I did forgive him. My boyfriend and I are living happily now. Thank you so much Dr Uwaifo his WhatsApp: +1(315) 277-2762 Email: [email protected] Website; https://druwaifospelltempl.wixsite.com/my-site-1
Reply
EVANS PHILIP
5/2/2024 08:55:19 am
Amazing Love Spell To Get Back With your Partner and Fix Your Broken Relationship WHATSAPP+2349161779461
Reply
Corie Johnson
5/3/2024 10:31:44 am
Hello my name is Corie Johnson from USA I want to tell the world about the great and mighty spell caster called PRIEST ELIJAH my husband was cheating on me and no longer committed to me and our kids when I asked him what the problem was he told me he has fell out of love for me and wanted a divorce I was so heartbroken I cried all day and night but he left home I was looking for something online when I saw an article how the great and powerful PRIEST ELIJAH have helped so many in a similar situation like mine he email address was there so I sent him an email telling him about my problem he told me he shall return back to me within 24hrs I did everything he asked me to do the nest day to my greatest surprise my husband came back home and was crying and begging for me to forgive and accept him back he can also help you contact
Reply
Olivia Higgins
5/8/2024 05:26:46 am
After I and my husband got married, we relocated to another city and we both got jobs and started working and living together happily. We never had any problems until a colleague of his started doing all she can to get my husband’s attention. I never knew all along what was going until he started sleeping out and making excuses. Things got out of control and he eventually stopped attending to my needs. I knew at that point I needed help so I contacted Dr Isikolo and explained everything to him. He told me all that has been going and promised to fix the problems for me which he did. He cast a love reunion spell for me which reunited i and my husband and he started being the man I always loved him to be just after 48 hours Dr Isikolo worked for me. We are both happy now and it would not have been possible if not for Dr Isikolo. Text him on WhatsApp via: +2348133261196 or visit his page (https://isikolo-temple.com).
Reply
Andrew Beckett
5/9/2024 05:01:16 am
I and my wife had a misunderstanding which led to a huge fight and she left home and returned back to her fathers house. I let my emotions got the best of me and stayed permanently away from her. Things grew worse when she started seeing another man and I never knew about it. I tried fixing the problem and getting her to return back home and she never came back. I later found out all that has been going on and decided to seek help to fix my marriage with her which made me contact Dr Isikolo. Just as expected he worked for me and the problem was fixed and I am reunited with my wife. She returned back home just after 48 hours as promised by Dr Isikolo. I am forever indebted to him for fixing the problem I had in my marriage. kindly contact him for fast and urgent Help, email him: [email protected] or WhatsApp him on: +2348133261196 or check his page https://isikolo-temple.com
Reply
Corie Johnson
5/9/2024 01:25:51 pm
Hello my name is Corie Johnson from USA I want to tell the world about the great and mighty spell caster called PRIEST ELIJAH my husband was cheating on me and no longer committed to me and our kids when I asked him what the problem was he told me he has fell out of love for me and wanted a divorce I was so heartbroken I cried all day and night but he left home I was looking for something online when I saw an article how the great and powerful PRIEST ELIJAH have helped so many in a similar situation like mine he email address was there so I sent him an email telling him about my problem he told me he shall return back to me within 24hrs I did everything he asked me to do the nest day to my greatest surprise my husband came back home and was crying and begging for me to forgive and accept him back he can also help you contact
Reply
Trudy Morris
5/11/2024 05:08:54 am
I never knew I could get my fiancé back to me until I contacted Dr Isikolo who helped me. I had a terrible misunderstanding with my man and we went different ways. I was down emotionally and knew not what to do to help the situation. So I got to know about Dr Isikolo. I contacted him and got him to help with my problems. He told me all that I needed to know and understood and I complied with procedures and he eventually fix the problem for me and now I and my fiancé are back together and I know we will get married soon. It won’t have been possible if Dr Isikolo didn’t help me as promised. The result of his work surely manifest after 48 hours and it 100% guaranteed. Its visible for me to see the effect of the result of everything he did for me and truly the love and affection between i and my fiancé is restored back fully and it gladdens my heart that i didn't loose him to anyone out there. He can as well help you if you reach out to him now. Text him on WhatsApp him on +2348133261196 or for more info, check his page (https://isikolo-temple.com)
Reply
Leon Hader
5/13/2024 09:21:11 am
I Have At Last Located A Trustworthy Cyber Expert Who Deals With Lost Bitcoin Troubles contact Lost Recovery Masters
Reply
Corie Johnson
5/15/2024 06:28:33 pm
Hello my name is Corie Johnson from USA I want to tell the world about the great and mighty spell caster called PRIEST ELIJAH my husband was cheating on me and no longer committed to me and our kids when I asked him what the problem was he told me he has fell out of love for me and wanted a divorce I was so heartbroken I cried all day and night but he left home I was looking for something online when I saw an article how the great and powerful PRIEST ELIJAH have helped so many in a similar situation like mine he email address was there so I sent him an email telling him about my problem he told me he shall return back to me within 24hrs I did everything he asked me to do the nest day to my greatest surprise my husband came back home and was crying and begging for me to forgive and accept him back he can also help you contact
Reply
Xavier Lukas
5/26/2024 03:47:09 am
Reply
Natasha Miller
5/31/2024 07:11:56 am
My husband whom I built my life with for 23 years left me and the kids without a word. Everything came crashing down on me and I reached out to our loved ones and no one could help. There came a time he filed for divorce even when we had no issues or ever fought over anything disastrous. Dr Isikolo came to my rescue and fixed the problem I had with my man. He reunited us back together again and he returned home to us. Indeed life is mysterious and I never thought I would experience what I did went through but all thanks to Dr Isikolo who worked for me and assured me of the positive results after 48 hours which indeed came to pass as he promised. He can as well fix your problems if you contact him now. Text him on WhatsApp him on +2348133261196 or visit his website (https://isikolo-temple.com)
Reply
Jason Oswald
6/2/2024 11:58:38 am
I lost my marriage after 2 years and it was a horrible experience for me. My wife left me and my son and everything happened beyond my control and I never knew few people around me engineered my wife and turned her against me just because I choose to build my family and focus more on it. I had to seek help because I know I did not do anything to have my marriage crashed. Dr Isikolo helped me and a lot was revealed to me on what transpired. He cast a love reunion spell that bonded my wife and I back together and the whole evil my family did against me was revealed. Am thankful that my home is back more happier than ever and all the appreciation goes to Dr Isikolo as he indeed fixed my problems just after 48 hours. Text him on WhatsApp him on +2348133261196 or visit his webpage (https://isikolo-temple.com)
Reply
Ashley Jason
6/5/2024 07:35:34 pm
My name is Ashley Jason from Canada, my husband and I have been quarreling almost all the time because he barely gives me attention. I didn't know that it was because he was seeing another woman. One day I went through his phone and found his chat with her and how he was always spending time with her so i confronted him and he told me that he has fallen out of love with me and he wanted a divorce I told him I don't want us to end our marriage because I love him so much, he didn't even listen to me he went to our room packed his clothes and left. I tried reaching out to him but to no avail, I cried and cried for weeks but nothing changed so I decided to search for ways to get my husband back online and I came across a testimony on how Dr. Great use his spell to reunite two lovers so i decided to contact him on WhatsApp and we spoke and he assured me that my husband will come back to me 24 hours after he finish casting the spell. And exactly 24 hours after I heard a knock on the door I went to open the door and I saw my husband on his knees begging me to accept him back again and he promised never to leave me or do anything to hurt me again. I let him plead for a few minutes before I accepted him again. I'm so happy today to tell the world that Dr Great is truly a man of his words. Do you have a problem with your marriage or relationship then contact Dr Great at
Reply
Ashley Jason
6/5/2024 07:36:04 pm
My name is Ashley Jason from Canada, my husband and I have been quarreling almost all the time because he barely gives me attention. I didn't know that it was because he was seeing another woman. One day I went through his phone and found his chat with her and how he was always spending time with her so i confronted him and he told me that he has fallen out of love with me and he wanted a divorce I told him I don't want us to end our marriage because I love him so much, he didn't even listen to me he went to our room packed his clothes and left. I tried reaching out to him but to no avail, I cried and cried for weeks but nothing changed so I decided to search for ways to get my husband back online and I came across a testimony on how Dr. Great use his spell to reunite two lovers so i decided to contact him on WhatsApp and we spoke and he assured me that my husband will come back to me 24 hours after he finish casting the spell. And exactly 24 hours after I heard a knock on the door I went to open the door and I saw my husband on his knees begging me to accept him back again and he promised never to leave me or do anything to hurt me again. I let him plead for a few minutes before I accepted him again. I'm so happy today to tell the world that Dr Great is truly a man of his words. Do you have a problem with your marriage or relationship then contact Dr Great at
Reply
Jessica Butler
6/8/2024 01:45:19 am
what a wonderful world we are living in, i still doubt this spell caster how he did it!!! I am so happy to let the whole world know how this powerful spell caster saved my marriage.Everything was going down the drain as my husband can not stop cheating on me with other women. It became used to always heating on me. I tried to make him stop, but I couldn't help the situation, the more I tried, the harder it became. At times we will fight and go apart for some months and we will come back again just because of our kids. One day a friend told me about this spell caster who helped her too, his name is Dr.oku, she said he uses white magic spells to solve spiritual problems. I decided to give it a try, I contacted him and he told me it will take just 2 to 3 days and I will see great changes in my husband. He actually cast a spell, believe me after 2 to 3 days of the spell, my husband was confessing different names of women he has slept with. He begged for forgiveness and never to try it again. From that day till now, my mind is at rest. My husband dislikes every other woman on earth except me. And am so happy to have him for myself alone.The spell caster’s contact is [email protected] you can also contact him on whatsapp +2347053113465
Reply
Jason Oswald
6/9/2024 04:48:05 am
I lost my marriage after 2 years and it was a horrible experience for me. My wife left me and my son and everything happened beyond my control and I never knew few people around me engineered my wife and turned her against me just because I choose to build my family and focus more on it. I had to seek help because I know I did not do anything to have my marriage crashed. Dr Isikolo helped me and a lot was revealed to me on what transpired. He cast a love reunion spell that bonded my wife and I back together and the whole evil my family did against me was revealed. Am thankful that my home is back more happier than ever and all the appreciation goes to Dr Isikolo as he indeed fixed my problems just after 48 hours. Text him on WhatsApp him on +2348133261196 or visit his webpage for more info about his works (https://isikolo-temple.com)
Reply
Olivia Higgins
6/12/2024 06:23:15 am
After I and my husband got married, we relocated to another city and we both got jobs and started working and living together happily. We never had any problems until a colleague of his started doing all she can to get my husband’s attention. I never knew all along what was going until he started sleeping out and making excuses. Things got out of control and he eventually stopped attending to my needs. I knew at that point I needed help so I contacted Dr Isikolo and explained everything to him. He told me all that has been going and promised to fix the problems for me which he did. He cast a love reunion spell for me which reunited i and my husband and he started being the man I always loved him to be just after 48 hours Dr Isikolo worked for me. We are both happy now and it would not have been possible if not for Dr Isikolo. Contact him if you need any help. text him on WhatsApp him on +2348133261196 or check his webpage (https://isikolo-temple.com)
Reply
Agata Winston
6/14/2024 05:45:37 am
My husband had the habit of always texting and fixing dates with his old friends including his exes. I never thought there was a problem with such until he became emotionally withdrawn from me and started acting abnormal towards me and my daughter. At this point I knew I needed help urgently because I never wanted to loose him. Dr Isikolo came to my rescue and the problem was fixed. One my husband’s ex vowed to ensure she takes him from him and started manipulating him to abandon me and my daughter which would have eventually happened if Dr Isikolo didn’t stepped in to help me. Just after 48 hours after fixing the problem, everything became amazing between me and my husband and now he has apologized for everything and we are good again. Contact Dr Isikolo and believe he will surely fix that problem for you. WhatsApp him on +2348133261196 or visit his only webpage (https://isikolo-temple.com) and see more for yourself.
Reply
Monica Albareda
6/15/2024 04:40:18 am
No one else can help you fix your relationship and love problems better than Dr Isikolo (https://isikolo-temple.com)
Reply
Jotasha Jones
6/16/2024 05:09:25 am
MY HUSBAND LEFT AND DR ISIKOLO GOT HIM BACK TO ME AND I AM AMAZED AND HAD TO SPREAD THE GOOD NEWS
Reply
Kimberly Williams
6/17/2024 05:31:19 am
THE POSSIBILITY OF GETTING YOUR EX PARTNER BACK IS GUARANTEED WITH DR ISIKOLO. CONTACT HIM NOW
Reply
Stacey Muller
6/21/2024 08:21:41 am
I met my husband while we were in college. We dated for quite a long time and cohabited and it was all love and bliss while both building our dreams. Things become very awkward when he travelled for a workshop and stayed for 6 months. He changed when he visited and i found out that he was seeing someone else in Ohio and he was serious with her. It broke me because i loved my husband so much and would do anything to have him back to myself alone. I had to reach out to Dr Ilekhojie who helped my aunt in the past and I complied with the instructions he gave me and repaired my marriage. My husband returned last week and i saw a message between him and this lady and he told her to stay away as he wants to focus on our marriage and start having kids. . All thanks to this great Dr Ilekhojie who i met through my aunt. Se his details here if you ever need his help. Email: [email protected] or contact his phone number +2348147400259
Reply
Charlene Harris
6/22/2024 05:44:17 am
WHEN LOOKING FOR A TRUSTWORTHY SPELL CASTER TO HELP YOU GET YOUR EX BACK, CONTACT DR ISIKOLO. HIS website (https://isikolo-temple.com)
Reply
Emily Cruff
6/24/2024 11:13:16 am
Everything was really tough on me after my divorce. I was devastated and couldn't even focus on work. I reached out to his friends and family to help us but despite great efforts from them, he did not listen. I was broken as i could not see myself with anybody else as my husband was my first and only love. So i had to seek help from Dr Ilekhojie who was recommended to me by a friend from work. He performed a reconciliation ritual which changed everything completely and it was overwhelming. His words is his bound and he never fails when he promises result. My husband suddenly called and told me that he wants to give our love another chance and it has been 4 months of love and happiness all over again. Don't bother seeking help elsewhere. Contact him now. His email: [email protected] or WhatsApp: +2348147400259
Reply
Jason Oswald
6/25/2024 05:15:58 am
I lost my marriage after 2 years and it was a horrible experience for me. My wife left me and my son and everything happened beyond my control and I never knew few people around me engineered my wife and turned her against me just because I choose to build my family and focus more on it. I had to seek help because I know I did not do anything to have my marriage crashed. Dr Isikolo helped me and a lot was revealed to me on what transpired. He cast a love reunion spell that bonded my wife and I back together and the whole evil my family did against me was revealed. Am thankful that my home is back more happier than ever and all the appreciation goes to Dr Isikolo as he indeed fixed my problems just after 48 hours. Text him on WhatsApp him on +2348133261196 or get more info about his works on his web (https://isikolo-temple.com)
Reply
Andrew Beckett
6/28/2024 05:24:03 am
I and my wife had a misunderstanding which led to a huge fight and she left home and returned back to her fathers house. I let my emotions got the best of me and stayed permanently away from her. Things grew worse when she started seeing another man and I never knew about it. I tried fixing the problem and getting her to return back home and she never came back. I later found out all that has been going on and decided to seek help to fix my marriage with her which made me contact Dr Isikolo. Just as expected he worked for me and the problem was fixed and I am reunited with my wife. She returned back home just after 48 hours as promised by Dr Isikolo. I am forever indebted to him for fixing the problem I had in my marriage. kindly contact him for fast and urgent Help, Text or call him on WhatsApp: +2348133261196 or check his page (https://isikolo-temple.com)
Reply
Aceline Carmen
6/30/2024 08:49:03 pm
I lost my husband to a lady abroad when he went to work in the same region where she lives. I never knew all that happened till a friend of mine sent me photos of both together and it was known to me after then that it was the reason why my husband grew cold towards me and left me behind. My husband was hypnotized I knew everything when I contacted Dr Ilekhojie when I searched for help and found none. He assured me of his return and having our love and happiness restored back which he did and the result started manifesting within 3 days. Now I have my husband back and I can't thank Dr Ilekhojie enough for his honesty and support. Just text him via WhatsApp +2348147400259 or email him via: [email protected]
Reply
Arlene Brown
7/2/2024 05:40:01 am
It gladdens my heart to be out here to say a word of thank you to Dr Isikolo.
Reply
In today's digital age, navigating the online landscape can sometimes feel like trekking through a treacherous wilderness. Lately, I found myself ensnared in a web of deceit spun by a group of frvudsters, leaving me feeling helpless and devastated. However, amidst the chaos, I stumbled upon a beacon of hope – COIN RECLAIM SERVICE a recovery agency that would become my saving grace.
Reply
Ferdinand Witter
7/4/2024 05:09:47 am
The marital crisis I was going through came to and end when Dr Isikolo got involved. Just like every other couples out there, we had our differences and I ensure I did my best to lead her right, provide for her and my kids and also protected them. We both made sacrifices to ensure we survived the union until she started acting up and deliberately had so many fights with me. The home became unpleasant for everyone else including my children. She was being manipulated by a friend who had been divorced and wanted to also ruin my marriage. I had to contact Dr Isikolo and he responded and did his best to end the issues. He restored the love and connection between us and I can tell now that whatever illusion my wife was under has been taking away and she is a better woman now. The result of what Dr Isikolo did for me that manifested after two days was what amazed me. I and my household remain grateful. I appeal to anyone who needs help to fix their relationships and marital problems to contact Dr Isikolo because the solution is sure. His website (https://isikolo-temple.com) or text him on WhatsApp him on +2348133261196
Reply
Paul Van Blom
7/6/2024 12:58:44 am
WHAT TO DO AFTER GETTING SCAMMED ONLINE GO TO LOST RECOVERY MASTERS
Reply
Maria Schaeffler
7/6/2024 09:28:42 am
I feel so blessed again in my marriage after Doctor Oku brought back my husband that separated with me for a good 3 months. Even though I have mouths all over my body, it won't be enough to thank Doctor Oku for his help in my life. My husband separated with me for 3 months and has been in pain and agony without him. So, I searched for help everywhere but nothing worked out, not until I meant Doctor Oku who I contacted online. I explained my situation to him and he promised that my husband will get back to me within 48 to 72 hours as long as my heart still beats for him. I believed in him and he prepared a spell for me and my husband called me exactly when Doctor Oku said. He pleaded and said he needs me back and now we are living happily again for the past 9 months. Everyone out there reading my article that needs help should contact him... Email: [email protected] or whatsApp him +2347053113465
Reply
Love Spells
7/6/2024 11:05:56 pm
Dr. Salem thank you so very much for helping to reunite me and my girlfriend! I didn’t think we would ever be able to work things out with all that had happened between us. But you wouldn’t let me be negative and you really did get her back for me! Thank you again so much! We are happy and planning a vacation to celebrate our engagement. Without you and your help, I know this would not have been possible. E-mail: [email protected]
Reply
Emma Kirby
7/7/2024 07:10:51 am
Earlier this year, I had a terrible fight with my husband and he had no choice but to leave the house and i assumed he was just anger that made him left. After few days, i couldn't contact him or get to know where he was. I waited and waited but he never returned or called me. I was filled with pain and remorse over what happened. I tried all i could to get him back but to no avail until i contacted Dr Ilekhojie who came to my rescue. He did his work perfectly to reunite us and my husband who did not want to return, called exactly after 48 hours just as the Dr promised. His contact Email [email protected] or Whatsapp only +2348147400259
Reply
CHIEF DR Sambola HERBAL THERAPY
Reply
Christine Allen
7/9/2024 05:11:33 am
Hi peeps. My name is Christine Allen and I have had tough and horrible experiences in my past relationships and I indeed waited till I met my husband and after we met, we fell in love and got married. After two years of our Union, he changed and started acting weird and eventually left me and our son. I Did all I could to get him back but all was fruitless. I came in contact with the comments and what everyone was saying about Dr Isikolo. I reached out to him and he responded and gave me his best effort and support to make my marriage work again. He was the one who made it known to me that my husband was taken from me by another woman and he cast a love reunion spell that reunited us back together and he came back home to me and my boy. Indeed no one out there has lied about Dr Isikolo and his good works. My husband came back home 48 hours after he did the work for as promised. Reach out to him now and be assured he will help you. You will have to checkout his page (https://isikolo-temple.com) or text him on WhatsApp via: +2348133261196
Reply
stephen
7/10/2024 09:59:53 am
HOW MANY BITCOINS ARE PERMANENTLY LOST? DO YOU KNOW?
Reply
Vivian Marcus
7/10/2024 11:36:19 am
Hello my name is Vivian Marcus from the United State, i'm so exciting writing this article to let people seek for help in any Break up Marriage and Relationship, Dr Kachi brought my Ex Boyfriend back to me, Thank you Sir Kachi for helped so many Relationship situation like mine to be restored, i was in pain until the day my aunt introduce me to Dr Kachi that she got her husband back with powerful love spell with help of Dr Kachi So i sent him an email telling him about my problem how my Boyfriend left me and cheating on me because of her boss lady at work i cry all day and night, but Dr Kachi told me my Boyfriend shall return back to me within 24hrs and to me everything he asked me to do the next day it was all like a dream when he text me and said please forgive me and accept me back exactly what i wanted, i am so happy now as we are back together again. because I never thought my Ex Boyfriend would be back to me so quickly with your spell. You are the best and the world greatest Dr Kachi. if you're having broke up Ex Lover or your husband left you and moved to another woman, You do want to get Pregnant do not feel sad anymore contact: [email protected] his Text Number Call: +1 (209) 893-8075 You can reach him Website: https://drkachispellcaster.wixsite.com/my-site
Reply
special divine
7/10/2024 07:52:19 pm
Reply
special divine
7/10/2024 07:52:55 pm
Reply
special divine
7/10/2024 09:23:52 pm
Reply
special divine
7/10/2024 09:26:31 pm
Reply
special divine
7/12/2024 01:58:42 am
Reply
Christopher Morris
7/12/2024 05:09:46 am
I met my wife when I was working and living in Alaska. Ever since we got married, it has been all good till she decided to go for a summit in another state where she met someone who became closer to her and eventually he eloped with her. All my efforts to get back home to me was all in vain and her family did their best to reunite us but nothing worked. Just like everyone else, I came in contact with Dr Isikolo and he eventually did wonders and now my wife is back to me. It was revealed that she was hypnotized by the guy who eloped with her. I am glad I never let my emotions get the best of me to have ended my marriage with her. Dr Isikolo is a strong spell caster and trust him when he says the results will manifest just after 48 hours. Contact him now if you need any help text him on WhatsApp: +2348133261196 or review his page for more info (https://isikolo-temple.com)
Reply
special divine
7/12/2024 08:27:32 am
Reply
Hilda Malen
7/12/2024 10:45:41 am
I was the last person on earth to accept the fact that spells exist or work not until I was referred to Dr Ilekhojie. He promised to help me reconcile with my partner. I had no other option than to give it a try because 3 months after the divorce, I was demoted at my place of work due to depression and lack of concentration. My life was draining away each day and i was confused on what to do. I was happy and enjoying my work but all of a sudden, i became miserable after the divorce because it was quick and a short process. Only Dr Ilekhojie gave me a way and i am happy i believe him. Just last week here, I was promoted back to my position and I’m here to share my own experience with this man called Dr Ilekhojie. In all situation there’s always a way out. Contact Dr Ilekhojie via TEXT OR WHATSAPP MESSENGER with: +2348147400259 and Email on: [email protected]
Reply
Natasha Miller
7/13/2024 04:57:53 am
My husband whom I built my life with for 23 years left me and the kids without a word. Everything came crashing down on me and I reached out to our loved ones and no one could help. There came a time he filed for divorce even when we had no issues or ever fought over anything disastrous. Dr Isikolo came to my rescue and fixed the problem I had with my man. He reunited us back together again and he returned home to us. Indeed life is mysterious and I never thought I would experience what I did went through but all thanks to Dr Isikolo who worked for me and assured me of the positive results after 48 hours which indeed came to pass as he promised. He can as well fix your problems if you contact him now. Text him on WhatsApp him on +2348133261196 or click on his webpage and read more about his works (https://isikolo-temple.com)
Reply
Stefania Slowik
7/13/2024 06:23:44 am
Good day everyone, I’m Stefania Slowik from Poland, my husband and I own Flower and Ornamental plants company, about two months ago we invested some part of our money into a cryptocurrency investment platform and made a total of $274,000 payment through bitcoins to this cryptocurrency platform not aware that it was all a scam, they kept asking us to make more payments into their platform and that was when we realized we have lost our investment. It was such a difficult time for us but while I was surfing the internet, I saw someone share a post about EVIL HACKERS RECOVERY, a reputable company that recovers stolen and lost funds, I didn’t hesitate to contact them and after providing all the information they needed, EVIL HACKERS RECOVERY was able to recover our money in 48 hours. We were shocked that such a thing could be possible but we are super excited we were able to recover our money all thanks to EVIL HACKERS RECOVERY. We are recommending EVIL HACKERS RECOVERY to everyone out there who have been defrauded too by these fake cryptocurrency investment platforms. Contact them at Email: recoveryevilhackers@ gmail.com or WhatsApp: +353899820359
Reply
Virginia Harold
7/14/2024 02:44:31 am
Advice to save your marriage and get your Ex Boyfriend/girlfriend back ,contact [email protected] or WhatsApp +14242983869 for Urgent effective love Spell to get ex lover back or save you marriage fast and his result is 100% guaranteed.
Reply
special divine
7/14/2024 08:18:10 pm
Reply
special divine
7/14/2024 08:19:05 pm
Reply
Jason Oswald
7/15/2024 05:13:38 am
I lost my marriage after 2 years and it was a horrible experience for me. My wife left me and my son and everything happened beyond my control and I never knew few people around me engineered my wife and turned her against me just because I choose to build my family and focus more on it. I had to seek help because I know I did not do anything to have my marriage crashed. Dr Isikolo helped me and a lot was revealed to me on what transpired. He cast a love reunion spell that bonded my wife and I back together and the whole evil my family did against me was revealed. Am thankful that my home is back more happier than ever and all the appreciation goes to Dr Isikolo as he indeed fixed my problems just after 48 hours. Call or text him on WhatsApp via: +2348133261196 his review his webpage (https://isikolo-temple.com)
Reply
Mirabela Hank
7/15/2024 07:59:19 am
My husband just woke up and decided our marriage was over. For a few months now, Hank and i have not been going well because he was having an affair with his assistant at work. I loved my husband so much and decided to stay and work on our marriage. In a short time, Hank stopped coming home and his close friend told me he has another apartment where he live with her. I was hurt and went on seeking for help because Hank was different from the man i married 10 years ago. Luckily, i found Dr Ilekhojie who promised to return my husband back to me. He performed a reconciliation spell and he returned back and now we are both happy again with our boys. If you have issues like mine, send Dr Ilekhojie an Email [email protected] or contact him on Whatsapp/Viber +2348147400259
Reply
Niki nicole
7/19/2024 01:35:12 am
EFFECTIVE AND POWERFUL SPELL CASTER ONLINE... This has really worked and I am proud to testify of it. I saw a post on how a lady got her man back by Dr. Happy . My Husband and I have been separated for 3 years and some months. Although I never believed in spiritual work I reluctantly tried him because I was desperate and his spell worked perfectly. My man is back and now my relationship is now perfect just as Dr. Happy promised me when I contacted him for help . Getting your ex back permanently does not only bring back someone you love back, but it will also re-ignite your lover’s feelings for you to be as happy with that person as possible. My man now treats me like a queen and always says he loves me all the time. If you are going through difficulties in your relationship Email him for urgent help.
Reply
Niki nicole
7/19/2024 01:40:53 am
EFFECTIVE AND POWERFUL SPELL CASTER ONLINE... This has really worked and I am proud to testify of it. I saw a post on how a lady got her man back by Dr. Happy . My Husband and I have been separated for 3 years and some months. Although I never believed in spiritual work I reluctantly tried him because I was desperate and his spell worked perfectly. My man is back and now my relationship is now perfect just as Dr. Happy promised me when I contacted him for help . Getting your ex back permanently does not only bring back someone you love back, but it will also re-ignite your lover’s feelings for you to be as happy with that person as possible. My man now treats me like a queen and always says he loves me all the time. If you are going through difficulties in your relationship Email him for urgent help.
Reply
Merel Daan
7/19/2024 09:44:15 am
I was a cheat and my husband caught me several times. I tried fixing myself and each time I ended up cheating over and over again. I guess I didn't realize what he meant to me until he had left. I began to find a way to get him back but nothing seemed to work out perfectly until I came across an article about Dr Ilekhojie who helped a lot of people globally to get their relationships back. I made contact with him and he assured me that my husband will come back to me and we will reconcile. Surprisingly, Just as he promised, my husband returned and told me he had forgiven me and ask us to start over again. All thanks to Dr Ilekhojie, I have a second chance to make things better and i have sworn that I will be faithful to my husband. You can ask him for help. Whatsapp or Viber: +2348147400259 or Email: [email protected]
Reply
Olivia Higgins
7/20/2024 05:38:12 am
After I and my husband got married, we relocated to another city and we both got jobs and started working and living together happily. We never had any problems until a colleague of his started doing all she can to get my husband’s attention. I never knew all along what was going until he started sleeping out and making excuses. Things got out of control and he eventually stopped attending to my needs. I knew at that point I needed help so I contacted Dr Isikolo and explained everything to him. He told me all that has been going and promised to fix the problems for me which he did. He cast a love reunion spell for me which reunited i and my husband and he started being the man I always loved him to be just after 48 hours Dr Isikolo worked for me. We are both happy now and it would not have been possible if not for Dr Isikolo. Contact him if you need any help. text him on WhatsApp via: +2348133261196 or checkout his page (https://isikolo-temple.com)
Reply
Andrew Beckett
7/21/2024 05:12:41 am
I and my wife had a misunderstanding which led to a huge fight and she left home and returned back to her fathers house. I let my emotions got the best of me and stayed permanently away from her. Things grew worse when she started seeing another man and I never knew about it. I tried fixing the problem and getting her to return back home and she never came back. I later found out all that has been going on and decided to seek help to fix my marriage with her which made me contact Dr Isikolo. Just as expected he worked for me and the problem was fixed and I am reunited with my wife. She returned back home just after 48 hours as promised by Dr Isikolo. I am forever indebted to him for fixing the problem I had in my marriage. kindly contact him for fast and urgent Help, Review his website for more info (https://isikolo-temple.com) or WhatsApp him on: +2348133261196
Reply
Arlene Brown
7/23/2024 05:03:06 am
It gladdens my heart to be out here to say a word of thank you to Dr Isikolo.
Reply
7/23/2024 08:48:47 am
My journey from victim to victor serves as a testament to the resilience of the human spirit and the power of perseverance. To those who find themselves ensnared in similar predicaments, I offer this beacon of hope: recovery is possible, even when the odds seem insurmountable.In closing, I extend my heartfelMy recent encounter with SWIFT SPY ASSETS RECOVERY marks a pivotal chapter in my life, one fraught with deception, hope, and ultimately, redemption. It began with what seemed like a promising investment opportunity but quickly unraveled into a sophisticated scam that left me reeling. It all started innocuously enough on the Telegram app, where I was lured into investing in what purported to be stocks of tech giants like Amazon and Apple. The scammers convinced me to download MetaTrader and Trust Wallet, tools that seemed legitimate for managing investments and cryptocurrency transactions. Little did I know, these were mere props in an elaborate scheme designed to defraud unsuspecting investors like myself. Eager to capitalize on what appeared to be a lucrative venture, I began funding the trading app with substantial wire transfers, eventually amounting to over 180,000USD. Each transaction seemed to reinforce the illusion that my investments were thriving in the booming tech market. However, the truth was far more sinister. It wasn’t until I attempted to withdraw my supposed profits that I realized something was amiss. Communication from the scammers became sparse, and when I did manage to contact them, their promises grew increasingly hollow. It dawned on me then: I had fallen victim to a meticulously orchestrated scam, and my hard-earned money was now in the hands of faceless criminals. In a desperate bid for justice, I turned to the NYPD, armed with evidence of my transactions and a trail of deceit. However, after a month of investigation, their verdict was disheartening: crypto assets, once transferred, were virtually untraceable. I was devastated by the realization that traditional law enforcement channels seemed ill-equipped to tackle crimes of this nature.Despite the bleak prognosis, a glimmer of hope flickered within me. I refused to accept defeat and resolved to explore alternative avenues for recovery. It was during this exhaustive search that I stumbled upon SWIFT SPY ASSETS RECOVERY, a name that would soon restore my faith in the fight against cybercrime. With little to lose and everything to gain, I entrusted Cyber Tech Wizard with my case. Swiftly, they sprang into action, meticulously tracing the convoluted path of my funds across the digital ether. Their expertise and determination were evident as they navigated through the complexities of blockchain transactions and cryptocurrency protocols.In a remarkable turnaround, just 72 hours later, SWIFT SPY ASSETS RECOVERY delivered the news I had begun to believe was impossible: my funds were successfully retrieved and restored to my bank account. The sense of relief and vindication was overwhelming, contrasting starkly with the despair I had felt mere days before. My journey from victim to victor serves as a testament to the resilience of the human spirit and the power of perseverance. To those who find themselves ensnared in similar predicaments, I offer this beacon of hope: recovery is possible, even when the odds seem insurmountable. In closing, I extend my heartfelt gratitude to SWIFT SPY ASSETS RECOVERY for their unwavering support and unwavering commitment to justice. They did not only restored my financial losses but also renewed my faith in the pursuit of justice in the digital age. To anyone navigating the aftermath of a scam, remember this: there are allies in the fight for restitution, and no setback is insurmountable with the right allies by your side. hire them to work for you if fallen vitim with the following information. Email.. (swiftrecoveryservice006 AT gmail DOT com) or WhatsApp number: +1 (786) 684‑0501. Or Telegram: SWIFT_HACKING website at https://swiftspyassetsrecovery.com
Reply
special divine
7/23/2024 02:22:58 pm
Reply
special divine
7/23/2024 02:24:00 pm
Reply
Ferdinand Witter
7/24/2024 05:46:43 am
The marital crisis I was going through came to and end when Dr Isikolo got involved. Just like every other couples out there, we had our differences and I ensure I did my best to lead her right, provide for her and my kids and also protected them. We both made sacrifices to ensure we survived the union until she started acting up and deliberately had so many fights with me. The home became unpleasant for everyone else including my children. She was being manipulated by a friend who had been divorced and wanted to also ruin my marriage. I had to contact Dr Isikolo and he responded and did his best to end the issues. He restored the love and connection between us and I can tell now that whatever illusion my wife was under has been taking away and she is a better woman now. The result of what Dr Isikolo did for me that manifested after two days was what amazed me. I and my household remain grateful. I appeal to anyone who needs help to fix their relationships and marital problems to contact Dr Isikolo because the solution is sure. Text him on WhatsApp him on +2348133261196 or visit his webpage for more details (https://isikolo-temple.com)
Reply
Teddy Marcelino
7/26/2024 05:09:10 am
I almost lost my marriage when I watched my wife turned into a total stranger and left the kids and I. I was so furious knowing I had done everything possible to ensure I sustained my marriage as a father and husband. The terrible fights we had traumatized me and I couldn’t function properly as a man. I kept on trying to find out what made her did what she did which made me contacted Dr Isikolo. I was surprised to have found out that she was under a huge manipulation from a man who wanted to ruin my marriage with her and take her away from me. Dr Isikolo had to intervene and fixed the problem thereby ensuring she was rescued from the claws of the dark magic charm they used on her. Knowing that I was able to get my family together again with the help of Dr Isikolo gives me joy and I am forever thankful to him. His website for more details (https://isikolo-temple.com) or text him on WhatsApp via: +234-8133261196
Reply
Gina
7/26/2024 08:45:10 am
Good works deserves good recommendation, I appreciate the effort of Dr.Ogudugu for helping me to bring back my husband, All thanks to him. I was heart broken when my husband left me and moved to California to be with another woman. I felt my life was over and my kids thought they would never see their father again. I tried to be strong just for the kids but I could not control the pains that tormented my heart, my heart was filled with sorrows and pains because I was really in love with my husband. I have tried many options but he did not come back, until i met a friend that directed me to Dr.Ogudugu a spell caster, who helped me to bring back my husband after 24hours. Me and my husband are living happily together again, This man is powerful, you can contact him now. I will advice anyone that have relationship problem or marriage problem, financial Difficulty, court case problem contact Dr.Ogudugu now, Here his contact.
Reply
Christopher Morris
7/27/2024 05:41:59 am
I met my wife when I was working and living in Alaska. Ever since we got married, it has been all good till she decided to go for a summit in another state where she met someone who became closer to her and eventually he eloped with her. All my efforts to get back home to me was all in vain and her family did their best to reunite us but nothing worked. Just like everyone else, I came in contact with Dr Isikolo and he eventually did wonders and now my wife is back to me. It was revealed that she was hypnotized by the guy who eloped with her. I am glad I never let my emotions get the best of me to have ended my marriage with her. Dr Isikolo is a strong spell caster and trust him when he says the results will manifest just after 48 hours. Contact him now if you need any help. text him on WhatsApp +2348133261196 or check his webpage (https://isikolo-temple.com)
Reply
Leave a Reply. |
Details
Welcome to the Homebirth NSW Blog!
AuthorThere are various authors to our awesome Homebirth NSW blog, each article will specify the author. Archives
September 2022
Categories
All
|
















 RSS Feed
RSS Feed